One class of antimicrobial agent that is effective against bacteria is an antibiotic. Antibiotic drugs are widely used in the treatment and prevention of bacterial infections because they are the most effective type of antibacterial agent for battling these infections. They could eradicate the bacteria or stop them from growing.
Other types of antimicrobial types,
Antivirals
Antifungals
Antiparasitic
All these medicines are used to treat infections.
However, antibiotics’ incorrect usage causes some harmful situations it is called antibiotic resistance. Antimicrobial resistance, including antibiotic resistance, has been designated as a priority health issue by the World Health Organization (WHO). In 2023, researchers studied antimicrobial resistance and found some information.
- Bacterial antimicrobial resistance has been associated with 569,000 deaths in all 35 countries within the WHO Region of America.
- Antimicrobial resistance was found to be responsible for 141,000 deaths, or 11.1% of all deaths worldwide. When a person passes away due to an infection that was resistant to treatment, it is said that antimicrobial resistance (AMR) was the cause of the death.
- Bacterial respiratory infections (293,000 deaths), bloodstream infections (266,000 deaths), intra-abdominal infections (181,000 deaths), and urinary tract infections (80,000 deaths) were the four AMR-related infectious syndromes that were responsible for the majority of deaths in the area. They were responsible for 89% of bacterial infection-related deaths.
- Staphylococcus aureus, Escherichia coli, Klebsiella pneumonia, Streptococcus pneumonia, Pseudomonas aeruginosa, and Acinetobacter baumannii were the six deadliest pathogens. AMR-related deaths totaling 452,000 were caused by these pathogens.
- Dominica, the Dominican Republic, Guyana, Haiti, Jamaica, Suriname, and Venezuela had the highest newborn mortality rates. The nations with the lowest rates of AMR-related infant mortality were Antigua and Barbuda, Argentina, Canada, Chile, and Costa Rica.
The above data emphasize the importance of understanding antibiotic resistance under antimicrobial resistance. It is an important health topic in the world.
How to work antibiotics into a human body,
Antibiotics function by preventing essential bacterial processes. They eradicate bacteria or prevent them from proliferating. This aids in the immune system’s natural defense against the infection. Antibiotics come in a variety of varieties.
Based on the chemical formula/structure we can identify these major types of antibiotic classes.
| Antibiotic class | Relevant medicines |
| Beta Lactam antibacterials 1. Penicillins 2. Cephalosporins | 1. Penicillin, Amoxicillin 2. Cephalexin; Cefazolin; Cefdinir; Cefaclor; Cefepime |
| Macrolides | Azithromycin; Erythromycin |
| Tetracyclines | Tetracycline; Doxycycline |
| Sulfonamides and trimethoprim | Co-trimoxazole, Trimethoprim |
| Quinolones | Ciprofloxacin; Levofloxacin |
| Aminoglycosides | Streptomycin; Gentamicin |
| Lincosamides | Clindamycin |
| Azoles | Metronidazole; Tinidazole |
Antibiotic resistance,
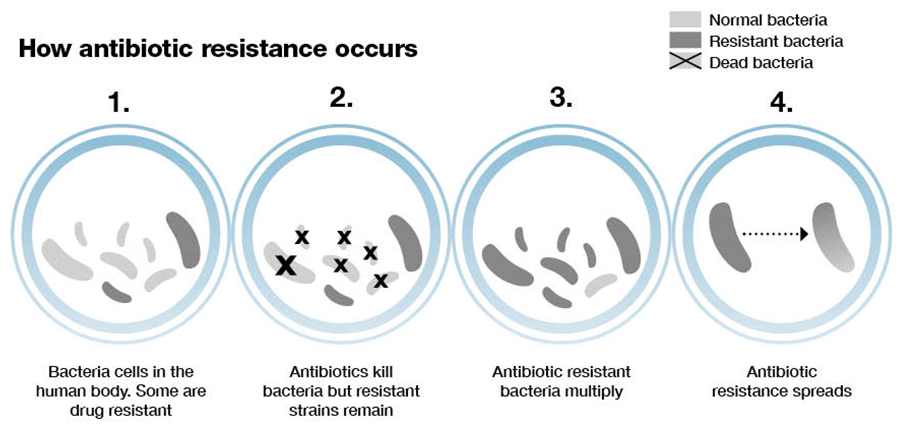
Bacteria develop antibiotic resistance when they adapt to defend against antibiotics. After coming into contact with an antibiotic, bacteria’s genes alter, or mutate, leading to the development of resistance.
The bacteria can now “resist” the antibiotic and live on thanks to these modifications. The antibiotic is no longer effective in eliminating the bacteria or preventing their spread. The antibiotic is no longer effective against the bacteria.
Additionally, bacteria that come into contact with one another may become resistant to antibiotics. Bacteria that are resistant to antibiotics can transmit their genes to other bacteria, creating new strains of resistant bacteria.
Bacteria have more opportunities to develop antibiotic resistance the more antibiotics are used.
The number of antibiotics available to doctors will decrease as more become ineffective against bacterial infections. The effectiveness of medications against many common infections may wane with time.
Causes for antibiotic resistance,
The main causes of antibiotic resistance in today’s world can be identified.
- Overprescription of antibiotics
- Patients not finishing the entire antibiotic course
- Poor infection control in healthcare settings
- Poor hygiene and sanitation
- Absence of new antibiotics being discovered

How to prevent antibiotic resistance
- How general public help to prevent antibiotic resistance
Properly hand wash – Millions of germs are continuously present in our bodies. Hand washing regularly can help ward off infections and sickness.
Identify the symptoms – Discover how to identify an infection’s early symptoms. If you suspect you have an infection, or if it is not improving or is becoming worse, see a healthcare provider.
Talk with healthcare providers – Discuss the rationale behind the antibiotic prescription, any potential side effects, and the duration of the medication’s use with your healthcare provider.
Learn how to use antibiotics in the right way – Understand when and how to use antibiotics appropriately. Antibiotics are not a cure-all for infections. Working with your healthcare provider, make sure you are getting the right antibiotic at the right dose for the right amount of time. Never insist on getting antibiotics if your doctor says they are not necessary.
Never share or use leftover antibiotics – Antibiotics should always be taken as prescribed by a doctor; do not stop taking them early or share any unused prescription medication. Never share or use leftover antibiotics.
Get vaccines – Obtain vaccinations Vaccinating against influenza once a year and keeping up-to-date records of all recommended vaccinations can help prevent illness.
- How healthcare professional helps to prevent antibiotic resistance
Prescribe antibiotics carefully – Need to follow the principles of antibiotic therapy;
In the first step, the doctor recommends the most suitable antibiotic treatment based on the most likely causative pathogen of infection together with other factors such as antibacterial sensitivity, the severity of the illness, age, disease status, history of any allergies, and the renal and the hepatic function of the patients.
Most viral infections are self-limiting (a disease that tends to go away on its own, without treatment) and should not be treated with antibiotics. In rare situations (eg-herpes simplex gingivitis and chicken pox pneumonia), antibiotics may be helpful to control secondary bacterial infection.
Appropriate samples should be sent for identification of the organism and sensitivity testing when possible before treating unexplained pyrexia. The knowledge of prevalent organisms and current sensitivity patterns is helpful when initiating therapy.
Selection of the dose of an antibiotic varies with the severity of the infection, the renal and hepatic function, and the age and weight particularly in children. An inadequate dose may lead to treatment failure and the likelihood of antibacterial resistance. It is important not to exceed the therapeutic dose particularly when antibiotics with a narrow toxic therapeutic ratio are used.
The route of administration is based on the severity of the infection. Most infections are treated with oral antibiotics although serious infections require intravenous administration.
The type of infection and how well the patient responds to treatment will determine how long the therapy takes. Oropharyngeal candidiasis and antibiotic-associated colitis are two examples of opportunistic infections that can result from prolonged therapy. Prolonged therapy is necessary for infections like endocarditis and tuberculosis.
Advice to patients clearly – Inform patients of the dangers and adverse effects of the antibiotics they are taking. Educate patients on the risks associated with antibiotic misuse and resistance.
Hand hygiene – Hand hygiene needs to before and after patient care.

Sources: